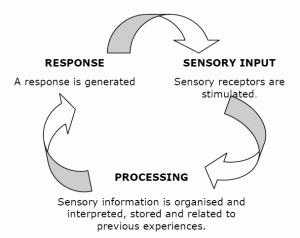
As discussed in my previous article, sensory integration dysfunction could seriously affect a child’s life if not diagnosed and targeted properly, thus, accurate diagnosis is of utmost importance.
Sensory integration dysfunction could be a tricky disorder, as symptoms may look similar to other disorders. One example of such disorders is Attention Deficit Hyperactivity Disorder, popularly known as ADHD. In both disorders, a child might present as hyperactive, or may face difficulty paying attention in class. Sensory integration dysfunction has also been often misdiagnosed as autistic spectrum disorder due to some shared symptoms, such as atypical activity level, or difficulty making friends.
These are few of many examples of inaccurate diagnosis of sensory integration dysfunction. This puts a big responsibility on parents in seeking the right kind of consultations and assessments, as well as critically appraising given answers to their child’s behaviours and difficulties.
Parents and professionals are usually alerted to the presence of sensory integration dysfunction by the child’s demonstrated self stimulatory or self soothing behaviours, through which the child attempts to regulate himself/herself, while hoping to feel more at peace with self and body.
If parents are in doubt that such a disorder may be affecting their child’s performance in daily life, they should seek the help of an occupational therapist who has a background in sensory integration assessment and intervention. A full assessment should be conducted by the occupational therapist to evaluate the reported difficulties and recommend further assessments or an intervention plan accordingly.
Several assessments are used by various therapists to confirm or rule out the presence of sensory integration disorder. One example of those tests are The Sensory Integration and Praxis Tests (Ayres, 1989), which were designed to assess various areas of performance in the child’s life which may be affected by this disorder. Other examples of assessment tools are the Sensory Profile Questionnaires. Those questionnaires were developed by Winnie Dunn. The different questionnaires were prepared to target several age groups, and several contexts; the Infant/Toddler Sensory Profile (Dunn, 2002a) is for caregivers of children of ages ranging between birth and 36 months, while the Sensory Profile -caregiver questionnaire- (Dunn, 1999a) is for caregivers of children ranging between three and ten years. The School Companion (Dunn, 2006a) is for school age children between three years and eleven years-eleven months, and is to be completed by teachers, while the Adolescent/Adult Sensory Profile (Brown and Dunn, 2002a) is self-completed and is for age eleven years and above.
Nevertheless, take note that a good therapist will not suffice by conducting a standardized assessment on your child, but will spend time with the child, play with him/her, as well as watch them playing or working on different tasks in more than one context.
The most important thing is to understand that no matter what the results of the assessment are, the given diagnosis never aims to give your child a label, but is instead considered the doorway to help him/her become better regulated, and accordingly plan and execute motor actions more accurately.
References:
Ayres, A. J. (1989). Sensory Integration and Praxis Tests. The United States of America. Los Angeles: Western Psychology Services.
Brown C.E and Dunn, W. (2002). Sensory Profile Adolescents/Adults (AASP). San Antonio, TX: Psychological Corporation.
Dunn, W. (1999). The Sensory Profile. San Antonio, TX: Psychological Corporation.
Dunn, W. (2002). Sensory Profile Infant/Toddler. San Antonio, TX: Psychological Corporation.
Dunn, W. (2006). Sensory Profile school companion. San Antonio, TX: Psychological Corporation.
Photo: Sensational Kids Occupational Therapy